 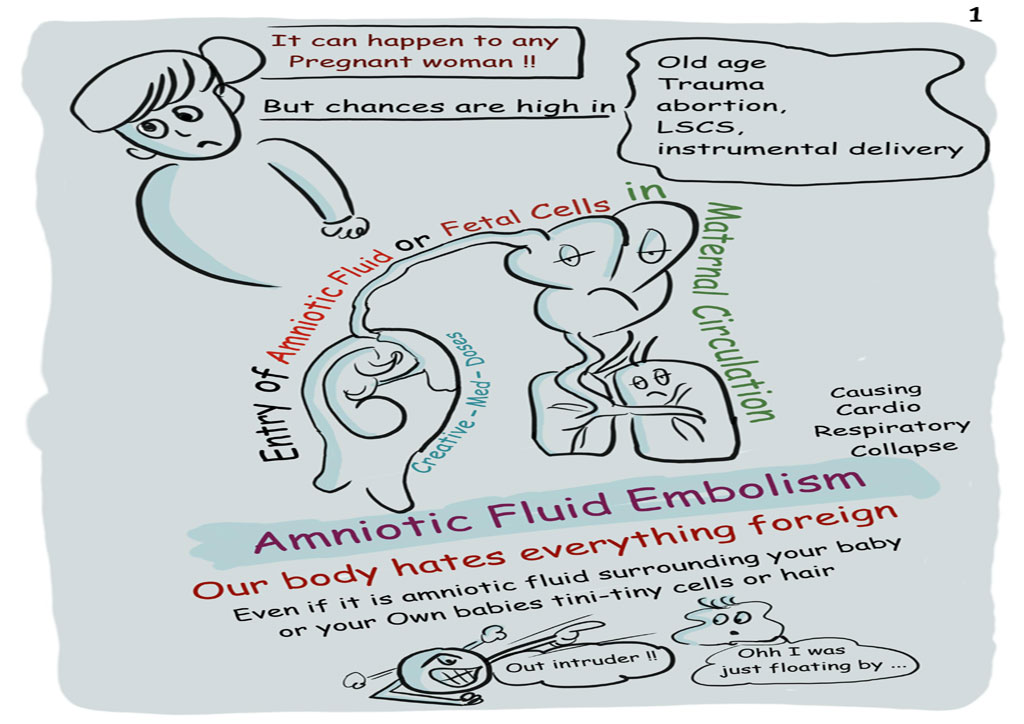
Therefore, the historical hypothesis was based on an obstruction of the pulmonary arteries from amniotic fluid or fetal debris. The common histopathological finding among these women was the presence of amniotic fluid debris in the pulmonary vasculature. It was later recognized as a syndrome in 1941 when Steiner and Lushbaugh reported autopsy findings of 32 women who died suddenly during childbirth. Although maternal morbidity and mortality remain high, advances in medical technology and improvements in obstetrical critical care and early diagnosis of AFE have improved outcomes.ĪFE was first described in the 1920s by J.R. Meyer. Management of women with AES is supportive and most often requires admission to an intensive care unit. There are no laboratory tests that confirm the diagnosis of AFE however, serum tryptase levels, complement levels, zinc coproporphyrin, and serum sialyl Tn (STn) may support the diagnosis. The diagnosis of amniotic fluid embolism is made based on clinical presentation. Risk factors often include advanced maternal age, induction of labor, cesarean delivery, operative vaginal delivery, placenta previa, and placental abruption. Abnormalities in the fetal heart tracing are almost always present. AFE presents as a sudden onset of hypoxia, hypotension, and coagulopathy during labor and delivery or in the immediate postpartum period. It is thought to be the result of a breach of the maternal-fetal barrier resulting in an abnormal maternal proinflammatory response. The pathophysiology of AFE is not completely understood. Given the rarity of this condition, there is a wide variation in reported incidence of amniotic fluid embolism. Amniotic fluid embolism (AFE) is a rare complication of pregnancy often resulting in catastrophic maternal and fetal outcomes. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
